Dentally for Canadian dental practices
Manage insurance claims and predeterminations with confidence using integrated CDAnet tools built specifically for Canadian workflows.
The challenge
Insurance admin tasks slow your team down. Manual tracking, missing attachments, rejected claims and unclear responses all add time and frustration to your day.
The solution
With Dentally’s CDAnet integration, you can submit claims electronically, track responses, and reconcile payments - all within one practice management solution.
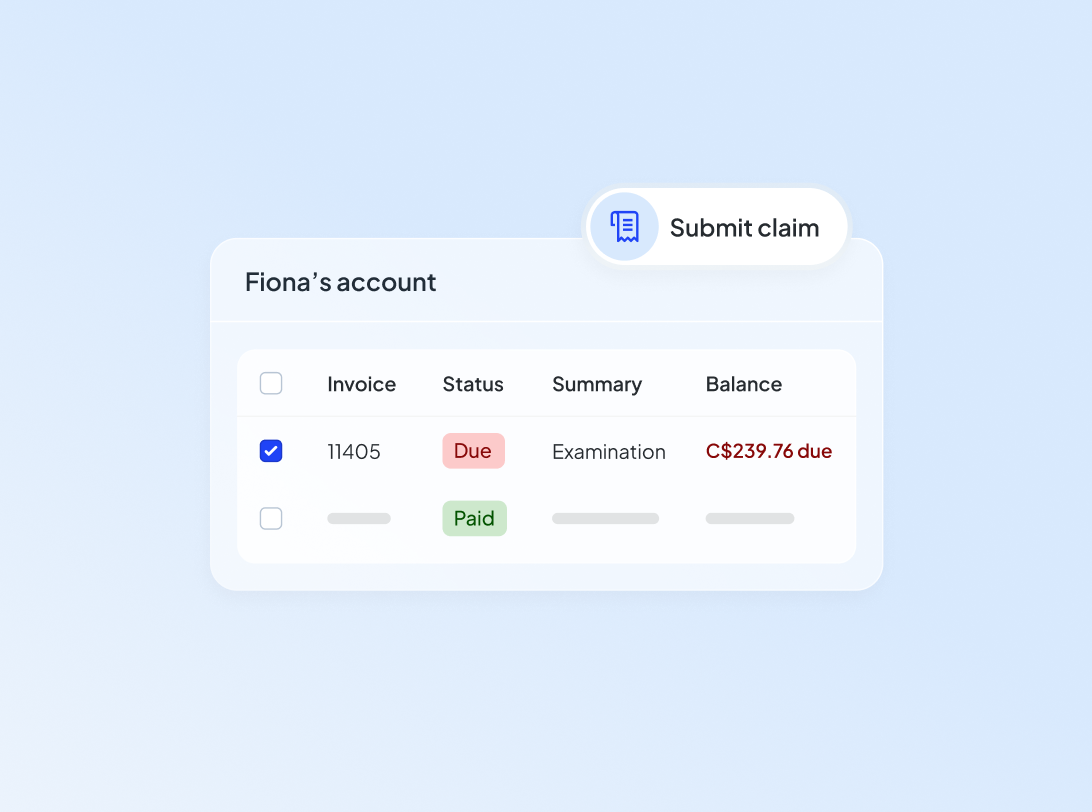
Designed specifically for Canadian workflows with CDAnet
Submit claims and predetermination directly to carriers, monitor responses in real time and manage everything from a simple Claims Management dashboard.

Real-time claim monitoring
Get instant feedback on transmission errors, track claim statuses and view insurer responses – all without leaving Dentally.


See insurance claiming in action
Discover how Dentally simplifies Canadian insurance processes, from submitting electronic claims to reconciling payments with clarity and confidence.
Benefits and outcomes
Centralized claims tracking
View pending, approved or returned claims at a glance. Filter by carrier or status, track responses, and reconcile payments efficiently from a single, easy-to-use dashboard.
Clear insight before treatment
Send predeterminations through CDAnet before treatment and receive insurer decisions back quickly, helping you provide patients with clear coverage estimates and fewer billing surprises.
Quick and reliable set-up
Configure CDAnet insurance carriers with guided set-up and built in validation, helping ensure claims are submitted correctly and reducing rejections from day one with Dentally.
Digital attachments made simple
Submit x‑rays, charts, and supporting documents electronically through CDAnet to eliminate manual forms, speed up processing time and minimize back and forth with insurers.

Simplify Canadian insurance
Our team will show you how Dentally and CDAnet work together to streamline submissions, reduce paperwork and give your practice greater control over claims management.